Childhood Trauma: Recognize Signs, Understand Effects, Find Practical Help
Childhood trauma doesn't always look dramatic. Sometimes it's a constant low-level worry, trouble sleeping, or a tightness you can't name. The CDC-Kaiser ACE Study showed adverse childhood experiences link to higher risk of health problems later in life. That doesn't mean you're broken—just that your brain and body reacted to danger and kept those reactions afterward.
First, how to spot it. Kids with trauma may have sudden anger, trouble focusing at school, or fear of being separated from adults. Teenagers can use substances, push people away, or act out to numb feelings. Adults who had a rough childhood often notice unexplained anxiety, relationship patterns that repeat, or chronic pain that doctors can't fully explain.
Why does it stick? Trauma changes stress systems. Your body learns to stay ready for threat. That helps during danger but creates wear-and-tear over years. Sleep, digestion, immune function, and mood can all be affected. That’s why therapy often looks at both emotions and physical health.
What helps right now? Start with small, concrete steps. Track triggers for a week: note situations where you feel flooded, what you thought, and how your body reacted. That data makes feelings less mysterious and gives a starting point. Build a short grounding routine—deep breaths, naming five things you can see, and three slow steps outside. Use it when you feel overwhelmed.
Professional paths that work. Trauma-focused therapies like EMDR and trauma-focused CBT have strong evidence. A trained therapist will move at a pace that feels safe and help you process memories and change reactions. Medication can help with symptoms like severe anxiety or sleep problems, but it usually works best alongside therapy.
Support without therapy. Peer groups, trusted friends, and support hotlines can be lifesaving. If you’re a parent, keep routines predictable for kids, notice sudden behavior changes, and seek help early. For teachers and health workers, simple screening questions—about sleep, safety at home, and mood—catch problems earlier.
Safety first: if you or a child are at immediate risk, call local emergency services or a crisis line now. If you're unsure where to start, make a single call to a mental health helpline and ask for a referral to a trauma-informed provider.
Common myths
Myth: time heals everything. Fact: unprocessed trauma can affect health for decades. Myth: only big events cause trauma. Fact: repeated neglect and emotional harm count. Recognizing myths helps you get the right care.
Finding a therapist
Check directories for 'trauma-informed' providers, read profiles, and ask about experience with EMDR or trauma-focused CBT. If cost is an issue, look for sliding scale clinics or university training clinics.
You deserve steady care and clearer days ahead — start today.
- 11 Comments
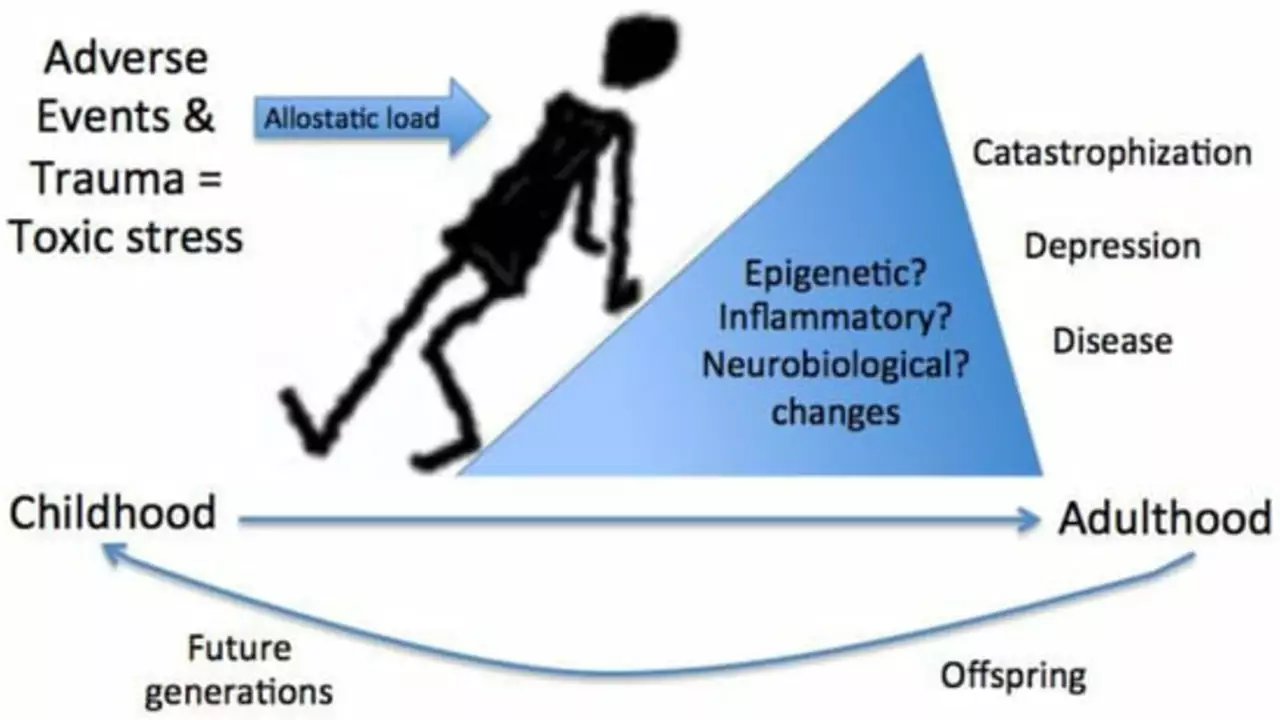
In my recent exploration, I've delved into the profound connection between childhood trauma and depression in adulthood. It seems that traumatic experiences during formative years can significantly increase the likelihood of depressive disorders later in life. Emotional, physical, or sexual abuse, as well as neglect, can leave deep psychological scars that may manifest as depression in adulthood. Additionally, the coping mechanisms children develop to survive such trauma can lead to mental health issues. This further emphasizes the critical importance of early intervention and support for children who have experienced trauma.
