Autoimmune Diseases: What to Watch For and How to Manage Them
Autoimmune diseases happen when your immune system attacks healthy tissue. That can cause joint pain, fatigue, rashes, fever, or organ-specific problems. Some conditions start suddenly; others creep up over months. Learning the common signs helps you get diagnosed faster and start the right treatment.
Spot the signs and take the first steps
If you have unexplained fatigue, joint stiffness (especially in the morning), persistent rashes, or repeated inflammation, put those symptoms on a short list. Track when they occur, what makes them better or worse, and any patterns — doctors love concrete details. Bring a full history of past infections, family autoimmune illnesses, and any meds or supplements you use. Ask your primary care doctor for basic blood tests (CBC, CRP/ESR, autoimmune panels) and a referral to a specialist, usually a rheumatologist or immunologist.
Don’t ignore flares. If pain or breathing problems spike, get medical help quickly. Mild flares are often managed with short medication adjustments and rest; severe flares can need urgent care. Keep a small symptom diary on your phone — a quick timestamped note beats vague memories at appointments.
Treatment basics, meds, and staying safe online
Treatment usually aims to reduce inflammation, control the immune response, and protect organs. Common medicines include steroids for short-term flare control, disease-modifying drugs like methotrexate or azathioprine, and biologics for targeted therapy. Hydroxychloroquine remains useful for lupus and some joint conditions. Each drug comes with monitoring rules — blood tests, liver checks, and infection screening — so stick to the schedule your doctor sets.
Thinking about buying meds online? Be careful. Always use pharmacies that require a valid prescription and show contact details and licensing. Ask for a pharmacist contact, check site reviews, and avoid offers that seem too cheap or skip prescription checks. If a site won’t verify your prescription or refuses to answer basic safety questions, walk away. For certain drugs (methotrexate, azathioprine, biologics), local supervision and lab monitoring are essential — these aren’t safe to self-manage.
Practical daily tips: get routine vaccines after talking to your doctor (live vaccines can be a problem on strong immune-suppressing drugs), practice good hand hygiene, avoid smoking, and aim for steady sleep and gentle exercise. Small lifestyle moves cut flares and make meds work better.
Finally, build a care team: a GP, a specialist, a pharmacist, and a trusted source for clear info. Keep copies of your test results, current meds, and allergies. When you’re informed and connected, you’ll spot problems earlier and make smarter choices about treatment and medication sources.
- 19 Comments
Explore how allergic disorders and autoimmune diseases share genetic, environmental, and inflammatory pathways, and learn practical steps to manage both conditions.
- 16 Comments
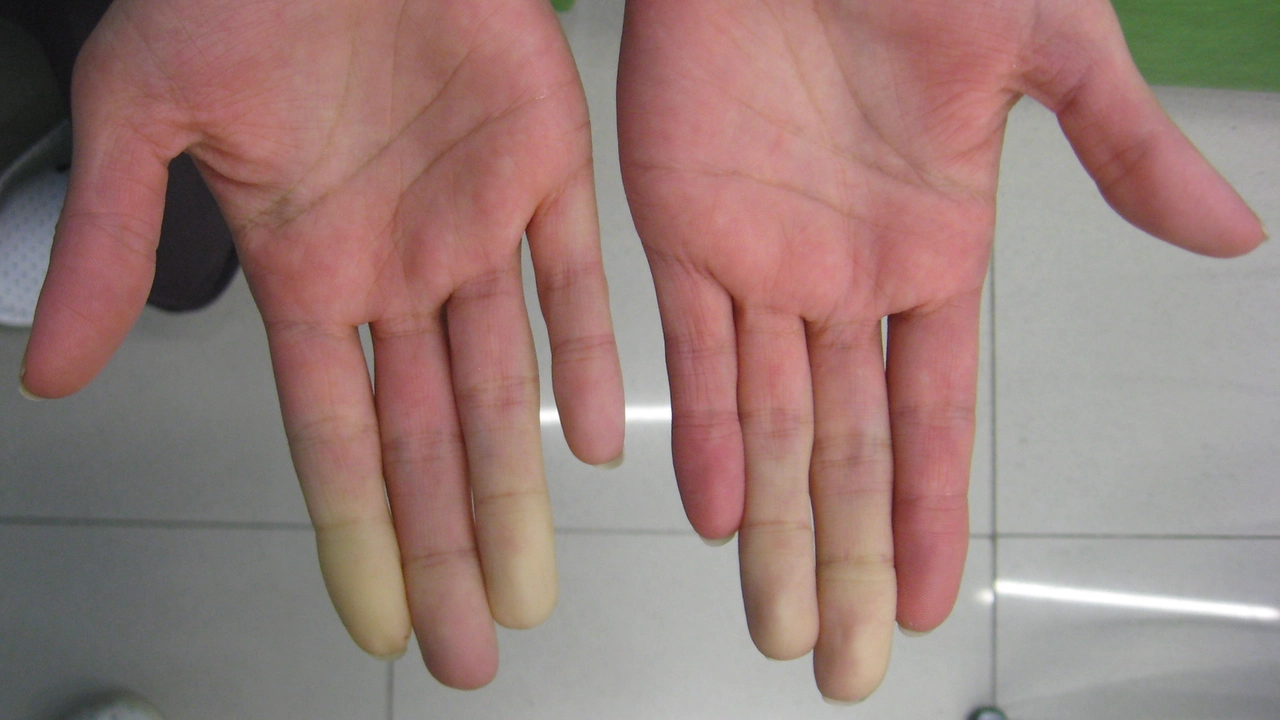
In exploring the link between Lupus and Raynaud's Phenomenon, I've found that these two conditions often occur together. Lupus, an autoimmune disease, can lead to Raynaud's, a condition causing some areas of your body to feel numb in response to cold temperatures or stress. While not all Lupus sufferers will experience Raynaud's, the presence of both can complicate treatment and management. It's essential to understand these connections and how they might affect those living with these conditions. Remember, being informed can help you navigate your health journey more effectively.
