Raynaud's Phenomenon — what it feels like and what to do right away
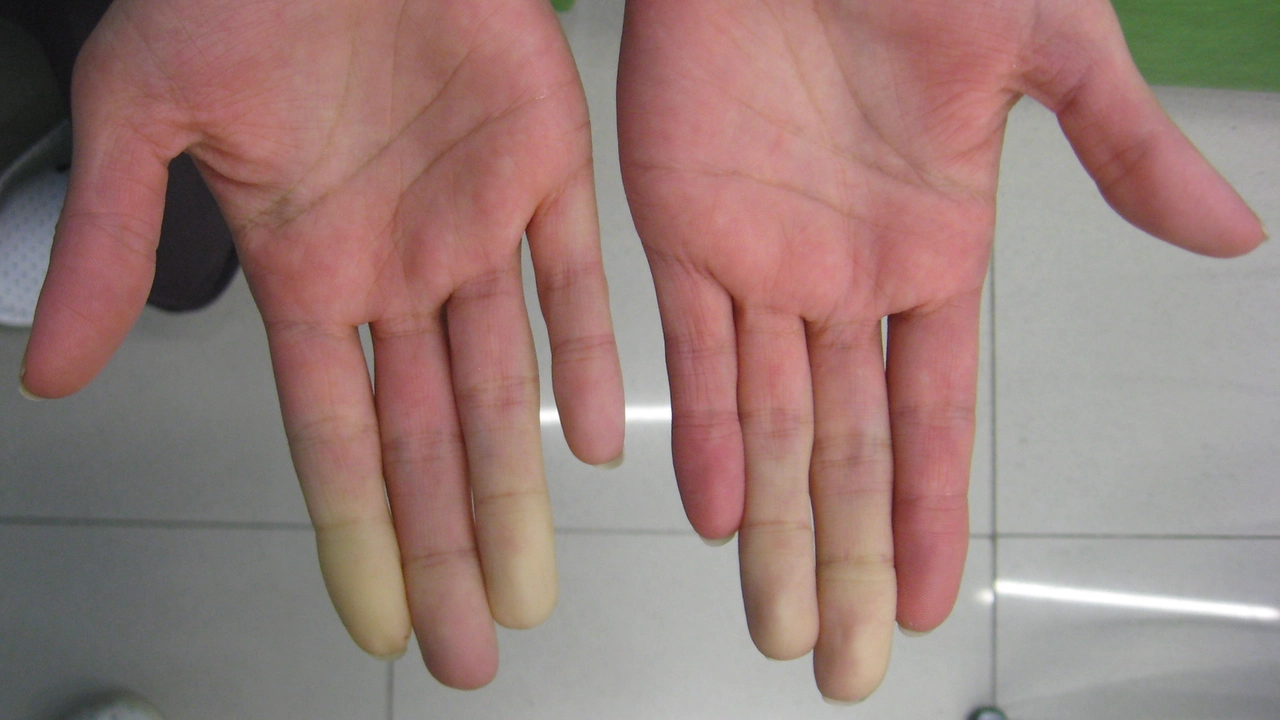
Does your fingers or toes turn white, then blue, then red when you get cold or stressed? That pattern is classic for Raynaud's phenomenon. It's a short-term spasm of the small blood vessels in the fingers and toes that cuts blood flow and causes numbness, pins-and-needles, and color changes. Attacks can be annoying or painful, but many people can reduce them with simple habits and a clear plan.
What causes Raynaud's and how to spot it
There are two common forms: primary Raynaud's, which happens on its own, and secondary Raynaud's, which comes from another condition (like an autoimmune disease) or from certain medicines. Triggers are usually cold exposure and emotional stress. Typical signs: fingers or toes that turn white, then blue, followed by redness as blood returns. Attacks last minutes to a few hours. If you get sores, persistent pain, or any tissue loss, see a doctor right away—those are warning signs of more serious disease.
Practical ways to manage attacks now and every day
Start with prevention. Keep your hands and feet warm: wear gloves, insulated boots, and use chemical hand warmers when needed. Layer clothing and protect your face in cold wind. Avoid sudden temperature changes—warm your car or shower before going outside. Stop smoking; nicotine narrows blood vessels and makes attacks worse.
Small behavior changes help a lot. Move your fingers and toes if you feel an attack starting—wiggling and shaking boosts blood flow. Place hands in warm (not hot) water to restore circulation. Manage stress with breathing exercises, short walks, or whatever calms you; stress is a common trigger.
Talk with your doctor about medicines if lifestyle steps aren't enough. Low-dose calcium channel blockers (like nifedipine) are commonly used to reduce attack frequency. Other options include topical nitrates or medications that improve circulation. If Raynaud's is secondary to another condition, treating that underlying issue changes the approach. Always follow a clinician's advice before starting any drug.
When your provider evaluates Raynaud's, they may check for signs of autoimmune disease, blood tests (ANA), or run simple vascular tests. In some cases a nailfold capillaroscopy is done to look at tiny capillaries near the nail for damage. Those tests help decide whether the condition is primary or secondary and guide treatment.
Practical tools people use every day: insulated gloves, heated socks, hand warmers, and avoiding vibrating tools that can worsen symptoms. If you travel to cold places, pack layers and plan warm breaks. For work that exposes you to cold, discuss accommodations with your employer.
If attacks are getting worse, causing ulcers, or limiting daily life, get medical help. Raynaud's can often be managed well, but early assessment matters—especially if an underlying disease might be involved. Small changes usually cut attacks by a lot, so start with warmth, stress control, and a quick chat with your doctor about next steps.
- 16 Comments
In exploring the link between Lupus and Raynaud's Phenomenon, I've found that these two conditions often occur together. Lupus, an autoimmune disease, can lead to Raynaud's, a condition causing some areas of your body to feel numb in response to cold temperatures or stress. While not all Lupus sufferers will experience Raynaud's, the presence of both can complicate treatment and management. It's essential to understand these connections and how they might affect those living with these conditions. Remember, being informed can help you navigate your health journey more effectively.
