Lupus: Practical Info on Treatment, Medications, and Safe Drug Access
Lupus can be confusing — it affects the immune system in unpredictable ways and needs a treatment plan that fits you. If you or someone you care about has lupus, this tag page collects clear, practical resources: medication guides, safe online buying tips, monitoring checklists, and alternatives when a drug isn't right.
Most people with lupus take one or more medicines to control flares and protect organs. Common drugs include hydroxychloroquine, methotrexate, azathioprine, corticosteroids, and biologics. Each has different benefits and side effects. Hydroxychloroquine often helps skin and joint symptoms and can lower flare risk; methotrexate and azathioprine are used for immune suppression; biologics target specific immune signals. Talk with your rheumatologist about which option matches your symptoms and test results.
Stopping or switching medicines needs a plan. For example, stopping hydroxychloroquine should trigger specific lab checks and symptom tracking — not a sudden stop. If a medication causes side effects, record what happened, when it began, and any lab changes. That record helps your clinician decide the safest next step and whether a slower taper or an alternative drug makes sense.
Worried about costs or where to buy your meds? Buying online is common but risky. Look for pharmacies that require a prescription, show a licensed address, and provide pharmacist contact info. Avoid sites that sell prescription meds without asking for a script. For drugs like methotrexate or biologics, pickup from a verified pharmacy or direct delivery from your health plan usually offers the safest route.
Watch lab tests and warning signs closely. Regular bloodwork — liver tests, blood counts, and kidney checks — is routine for many lupus drugs. Keep a simple checklist: drug name, last dose, date of last labs, and key symptoms to report (fever, new rashes, unusual bleeding, severe fatigue). Share that list with family or caregivers so someone else can notice changes.
Lifestyle and self-care matter alongside medicines. Sleep, stress control, sunscreen, and steady physical activity help reduce flares. Small steps like tracking your symptoms in a notes app, setting med reminders, and keeping water and sunscreen handy make daily life easier.
Use the articles linked under this tag to learn specifics: how to buy certain medications safely online, what side effects to expect, and practical monitoring tips when changing therapy. If you read something that concerns you, bring it to your clinician before making changes. Never adjust doses or stop immune-suppressing drugs without medical advice.
If you want a starting checklist to print or save: 1) Current meds and doses, 2) Recent lab dates and results, 3) Emergency contact and rheumatologist phone, 4) Pharmacy details and prescription status, 5) Notes on any new symptoms. That simple sheet speeds care during a flare or appointment.
Want more help? Browse the tag posts here for drug-specific guides — buying tips, side effect checklists, and monitoring plans. If an article mentions laws or online pharmacies, check the date and your local rules. When in doubt, call your pharmacy or clinic; a quick phone call can prevent serious mistakes.
- 16 Comments
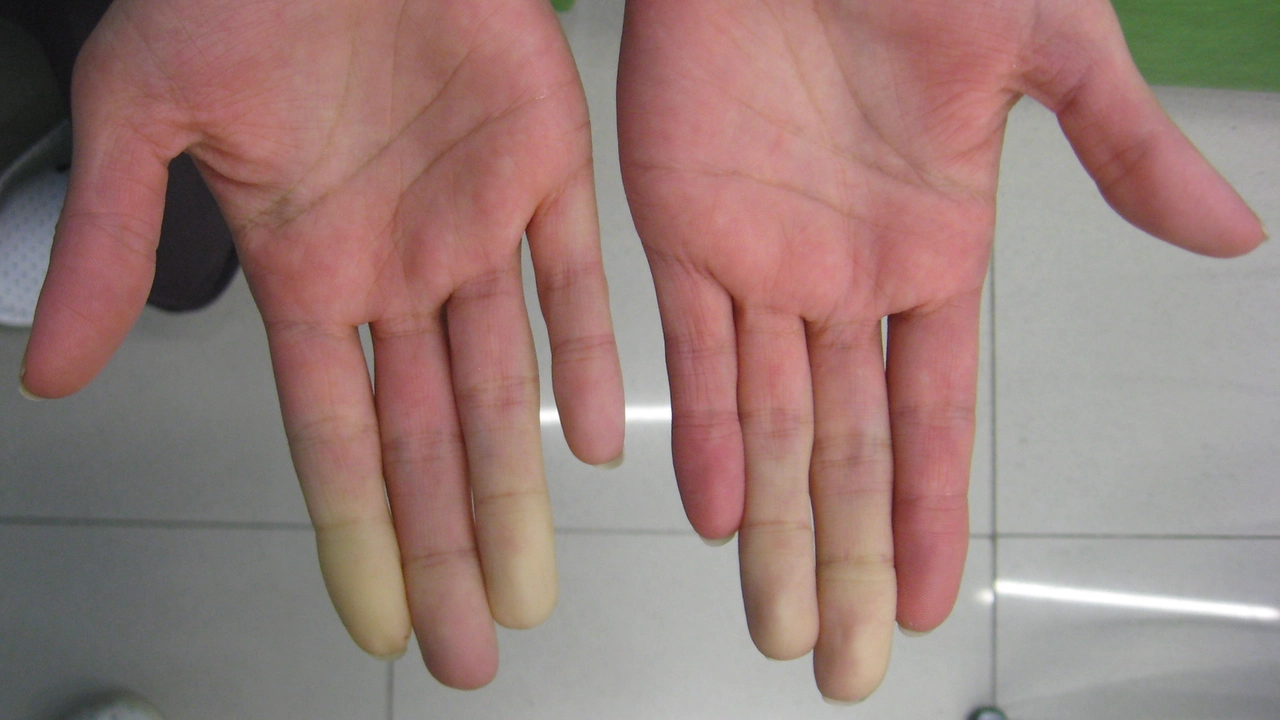
In exploring the link between Lupus and Raynaud's Phenomenon, I've found that these two conditions often occur together. Lupus, an autoimmune disease, can lead to Raynaud's, a condition causing some areas of your body to feel numb in response to cold temperatures or stress. While not all Lupus sufferers will experience Raynaud's, the presence of both can complicate treatment and management. It's essential to understand these connections and how they might affect those living with these conditions. Remember, being informed can help you navigate your health journey more effectively.
