Blood Pressure Control: Simple, Practical Ways to Lower Numbers
High blood pressure can sneak up on you. The good news: small, consistent changes and the right meds usually move your numbers in the right direction. This page gives clear, practical steps you can start using today—how to check your pressure at home, which drug types do what, and quick lifestyle moves that make a real difference.
Medication options
Medications are tailored to the person, but knowing the main classes helps you ask better questions. Calcium channel blockers like nifedipine (Procardia) relax blood vessels and work fast for some people. Diuretics—hydrochlorothiazide is common—help your body shed salt and water; alternatives include torsemide and spironolactone when different effects are needed. ACE inhibitors (eg, lisinopril) and ARBs (eg, losartan) protect the heart and kidneys and are often first-line. Beta-blockers slow the heart rate and help in certain conditions like angina or after a heart attack.
Side effects matter: nifedipine can cause flushing or swelling; thiazide diuretics may change potassium and sugar levels. If a medication causes bad symptoms, don’t stop suddenly—talk to your doctor or pharmacist about switching or adjusting doses. Pharmacists can screen for interactions and help you understand refill timing and generic options.
Practical daily steps
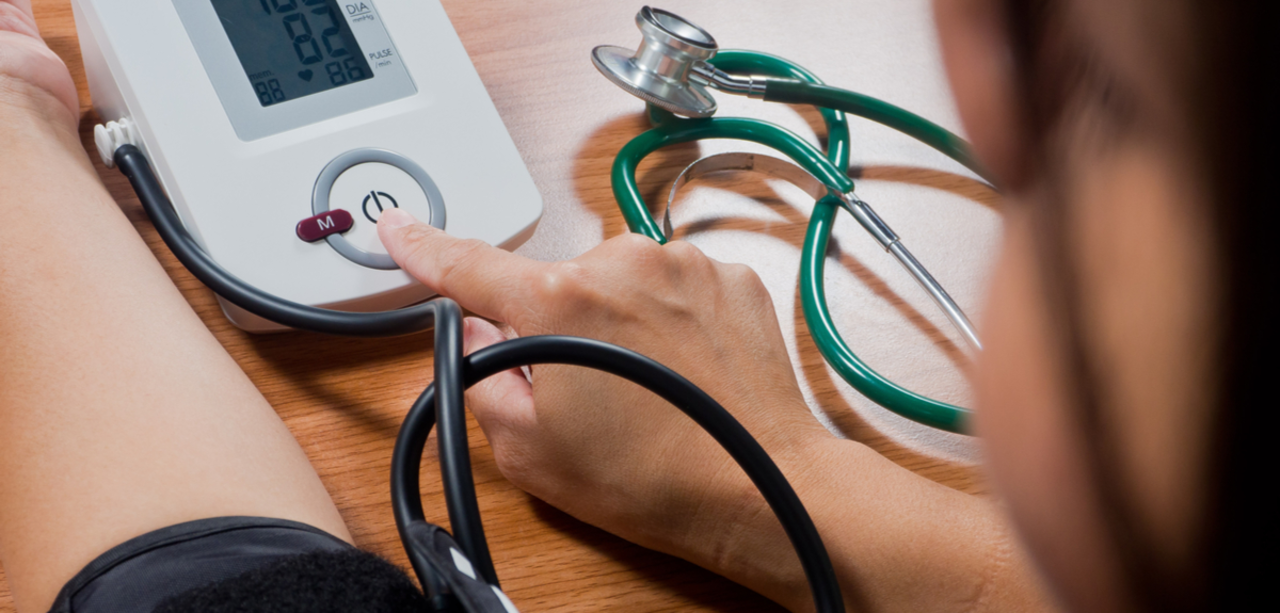
Measure correctly: use a validated upper-arm cuff, sit quietly for five minutes, take two readings one minute apart, and log the average. Check at the same times each day—morning and evening are common—and bring the log to appointments.
Cut sodium smartly: aim for under 2,000 mg a day if you can. Read labels, avoid canned soups and processed foods, and swap salty snacks for nuts or fruit. Move more: 30 minutes of brisk walking most days lowers blood pressure and helps weight control. Lose even 5% of body weight if you’re overweight—that often lowers readings.
Limit alcohol, sleep enough (7 hours is a good goal), and manage stress with simple tools—short walks, breathing exercises, or a hobby that helps you relax. Potassium helps some people lower pressure, so ask about foods like bananas, beans, and spinach—but check with your provider if you take potassium-sparing meds.
Stick with treatment: missing doses makes control harder. Use a pillbox, set phone reminders, and get refills early. If cost or side effects are a problem, your pharmacist can often suggest lower-cost generics or alternative schedules to discuss with your doctor.
If your readings stay high (consistently above 140/90 at home, or as advised by your clinician), or you get chest pain, shortness of breath, or sudden weakness, seek medical care. For everyday care, regular check-ins with your clinician plus smart home monitoring and these lifestyle steps will keep you moving in the right direction.
- 9 Comments
In my recent blog post, I discussed the relationship between Azilsartan and blood pressure control in patients with anxiety disorders. Azilsartan is an angiotensin receptor blocker (ARB) commonly used to treat hypertension. I found that there is growing evidence suggesting that this medication may be particularly beneficial for those suffering from anxiety disorders, as it has been shown to significantly reduce both systolic and diastolic blood pressure. Additionally, it may improve the overall cardiovascular health of these individuals, leading to a better quality of life. It's essential to consult with a healthcare professional before making any changes to your medication regimen, but it's certainly worth exploring the potential benefits of Azilsartan for those struggling with anxiety and high blood pressure.
